India implemented a national lockdown to
contain the spread of COVID-19 pandemic. The lockdown was announced suddenly,
and without a prior warning to give time to people to prepare for it. The
suddenness with which lockdowns were implemented does not seem to have been
part of any plan but a reflection of the lack of planning. On March 16, the
Prime Minister asked people across the country to self-quarantine just for a
day, on March 22. In the evening of March 22, he announced that some districts
were being locked down. And then on the evening of March 23, he announced a
complete, 21 day, country-wide lockdown starting midnight of March 24. As we
write this, there is news that it is being extended for another two weeks,
until April 30.
contain the spread of COVID-19 pandemic. The lockdown was announced suddenly,
and without a prior warning to give time to people to prepare for it. The
suddenness with which lockdowns were implemented does not seem to have been
part of any plan but a reflection of the lack of planning. On March 16, the
Prime Minister asked people across the country to self-quarantine just for a
day, on March 22. In the evening of March 22, he announced that some districts
were being locked down. And then on the evening of March 23, he announced a
complete, 21 day, country-wide lockdown starting midnight of March 24. As we
write this, there is news that it is being extended for another two weeks,
until April 30.
Response to Covid-19 necessitates social
distancing, testing, quarantine or isolation as necessary means to slow down or
control the spread. Even though complete lockdown of all economic activities as
an effective means to achieve the above is arguable, this article focuses on an
unfolding socio-economic crisis in the country as a vast majority of workers,
who are employed in the informal economy, found themselves robbed of their
means of livelihood with nothing to fall back on. As enterprises and
establishments downed their shutters and the economic activity came to a
grinding halt, small producers and workers across all sectors found themselves
robbed of their livelihood, and in many cases, stranded far away from their
families.
distancing, testing, quarantine or isolation as necessary means to slow down or
control the spread. Even though complete lockdown of all economic activities as
an effective means to achieve the above is arguable, this article focuses on an
unfolding socio-economic crisis in the country as a vast majority of workers,
who are employed in the informal economy, found themselves robbed of their
means of livelihood with nothing to fall back on. As enterprises and
establishments downed their shutters and the economic activity came to a
grinding halt, small producers and workers across all sectors found themselves
robbed of their livelihood, and in many cases, stranded far away from their
families.
The distress created by this sudden
imposition of a prolonged national lockdown has resulted a surge in distress
deaths. This surge, starting on March 25th, the first day of the national
lockdown, has continued unabated throughout the three weeks of the lockdown.
This article is an attempt to systematically examine the distress deaths caused
by the imposition of a prolonged country-wide lockdown without preparation and
planning. In this article, we refer to deaths because of COVID infections and
co-morbidity as infection deaths and deaths due to distress caused by
mitigation strategies as distress deaths.
imposition of a prolonged national lockdown has resulted a surge in distress
deaths. This surge, starting on March 25th, the first day of the national
lockdown, has continued unabated throughout the three weeks of the lockdown.
This article is an attempt to systematically examine the distress deaths caused
by the imposition of a prolonged country-wide lockdown without preparation and
planning. In this article, we refer to deaths because of COVID infections and
co-morbidity as infection deaths and deaths due to distress caused by
mitigation strategies as distress deaths.
The data on distress deaths has been
compiled by us using newspaper and online reports with the help of many friends
and colleagues. The dataset is regularly updated and is available at https://coronapolicyimpact.org.
Along with us, a few other groups active on social media are also compiling
similar data. All these datasets are public and provide the original source of
news for each case. We cross-verify our dataset with other similar lists to
ensure that we do not miss anything that others have identified and we do not
double count any cases.
compiled by us using newspaper and online reports with the help of many friends
and colleagues. The dataset is regularly updated and is available at https://coronapolicyimpact.org.
Along with us, a few other groups active on social media are also compiling
similar data. All these datasets are public and provide the original source of
news for each case. We cross-verify our dataset with other similar lists to
ensure that we do not miss anything that others have identified and we do not
double count any cases.
We would like to highlight that, despite
our best efforts, there is a high possibility that a significant number of
distress deaths go unrecorded. There are at least three reasons for this.
First, unlike the cases of COVID-19 infections, there is no system of official
recording of distress deaths. Secondly, not every death –– particularly of poor
people dying in remote villages –– is reported in the media. Apart from the
fact that media might not give space to every single death, coverage might also
be low because, under lockdown, the reach of the media has become restricted. Thirdly,
of what is covered in the media, bulk of the reports are in vernacular press.
Among the various people and groups that are tracking these news, we have been
able to cover English, Hindi, Tamil, Kannada, Telugu, Malayalam and Gujarati
press, but are unable to cover many others. Also even when somebody among us
can read a particular language, we cannot rule out the possibility that,
despite all the efforts, some reports are missed. It must also be noted that
there is sometimes a lag in the reporting of these deaths and our finding these
reports. As a result, the problem of under-counting is somewhat accentuated in
the most recent data and the data for the most recent days should be
interpreted with extra caution. Finally, some cases of suicides and deaths,
although related to the lockdown, may not be reported as such. Unless the
report specifically draws the connection with COVID and lockdown-related
issues, we do not include it in the database. This may result in exclusion of
some cases.
our best efforts, there is a high possibility that a significant number of
distress deaths go unrecorded. There are at least three reasons for this.
First, unlike the cases of COVID-19 infections, there is no system of official
recording of distress deaths. Secondly, not every death –– particularly of poor
people dying in remote villages –– is reported in the media. Apart from the
fact that media might not give space to every single death, coverage might also
be low because, under lockdown, the reach of the media has become restricted. Thirdly,
of what is covered in the media, bulk of the reports are in vernacular press.
Among the various people and groups that are tracking these news, we have been
able to cover English, Hindi, Tamil, Kannada, Telugu, Malayalam and Gujarati
press, but are unable to cover many others. Also even when somebody among us
can read a particular language, we cannot rule out the possibility that,
despite all the efforts, some reports are missed. It must also be noted that
there is sometimes a lag in the reporting of these deaths and our finding these
reports. As a result, the problem of under-counting is somewhat accentuated in
the most recent data and the data for the most recent days should be
interpreted with extra caution. Finally, some cases of suicides and deaths,
although related to the lockdown, may not be reported as such. Unless the
report specifically draws the connection with COVID and lockdown-related
issues, we do not include it in the database. This may result in exclusion of
some cases.
An additional risk comes from the
distortion of reporting across media sources: in some cases, details including
names, dates and ages related to the same incident are reported differently in
different reports creating the possibility of double counting. Avoiding such errors
is a challenge and requires special care.
distortion of reporting across media sources: in some cases, details including
names, dates and ages related to the same incident are reported differently in
different reports creating the possibility of double counting. Avoiding such errors
is a challenge and requires special care.
In addition to our dataset on distress
deaths, the article uses data on infection deaths from the India COVID-19
Tracker website (https://www.covid19india.org). Official data on
number of deaths due to COVID-19 infections are provided in daily bulletins
released by the Ministry of Health and Family Welfare. COVID-19 Tracker website
combines these with State-level information, which is usually more update and more
detailed. The team working for this website compiles all the information and
verifies it.
deaths, the article uses data on infection deaths from the India COVID-19
Tracker website (https://www.covid19india.org). Official data on
number of deaths due to COVID-19 infections are provided in daily bulletins
released by the Ministry of Health and Family Welfare. COVID-19 Tracker website
combines these with State-level information, which is usually more update and more
detailed. The team working for this website compiles all the information and
verifies it.
It is worth mentioning that the data on
infection deaths could also be somewhat understated if all people dying with
flu-like symptoms are not tested for COVID-19 infection. A majority of
infection deaths take place because of co-morbidity (other diseases such as
diabetes or hypertension becoming aggravated because of COVID infection). It is
therefore possible that deaths of some people with other sicknesses, along with
flu-like symptoms, are recorded as deaths because of other problems (say, heart
failure) without them being tested for COVID-19 infections. While lack of
testing may cause some under-reporting, the extent of under-reporting in data
on deaths is likely to be less than in the data on COVID-19 infections. This is
because people with critical illnesses are more likely to go to hospitals, and
if they go to hospitals in a critical situation with flu-like symptoms, than
period with mild symptoms. As a result, the chances of getting tested would be
higher for people with critical illnesses.
infection deaths could also be somewhat understated if all people dying with
flu-like symptoms are not tested for COVID-19 infection. A majority of
infection deaths take place because of co-morbidity (other diseases such as
diabetes or hypertension becoming aggravated because of COVID infection). It is
therefore possible that deaths of some people with other sicknesses, along with
flu-like symptoms, are recorded as deaths because of other problems (say, heart
failure) without them being tested for COVID-19 infections. While lack of
testing may cause some under-reporting, the extent of under-reporting in data
on deaths is likely to be less than in the data on COVID-19 infections. This is
because people with critical illnesses are more likely to go to hospitals, and
if they go to hospitals in a critical situation with flu-like symptoms, than
period with mild symptoms. As a result, the chances of getting tested would be
higher for people with critical illnesses.
The most important finding from these
data is that the total number of COVID-related deaths are not merely deaths due
to infection but are also due to distress resulting from the manner in which
the lockdown was implemented. And these distress deaths are not a small number
and even though both infection and distress deaths may be understated, these
make the total number of deaths significantly higher.
data is that the total number of COVID-related deaths are not merely deaths due
to infection but are also due to distress resulting from the manner in which
the lockdown was implemented. And these distress deaths are not a small number
and even though both infection and distress deaths may be understated, these
make the total number of deaths significantly higher.
As per the information available at the
time of writing this article, the total number of recorded deaths associated
with the COVID-19 pandemic in India was 515. Of these, 334 were
infection deaths while 181 were distress deaths. Imposition of a prolonged lockdown without
planning has resulted in loss of livelihoods for a vast number of people and
created a whole range of other problems which had not been thought about
despite the fact that India had several months of time to prepare to deal with
the pandemic. In terms of recorded data, the number of distress deaths were
higher than number of infection deaths until April 6th after which the
infection deaths have tended to increase faster than the distress deaths.
time of writing this article, the total number of recorded deaths associated
with the COVID-19 pandemic in India was 515. Of these, 334 were
infection deaths while 181 were distress deaths. Imposition of a prolonged lockdown without
planning has resulted in loss of livelihoods for a vast number of people and
created a whole range of other problems which had not been thought about
despite the fact that India had several months of time to prepare to deal with
the pandemic. In terms of recorded data, the number of distress deaths were
higher than number of infection deaths until April 6th after which the
infection deaths have tended to increase faster than the distress deaths.
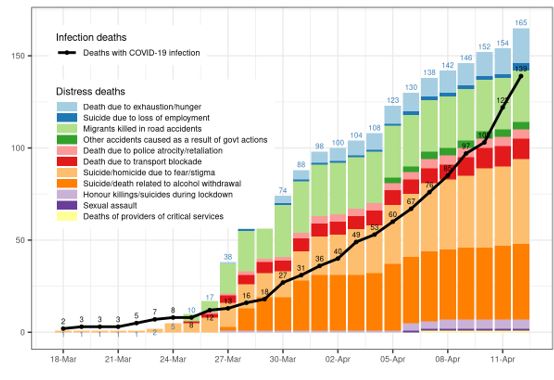
Figure
1. Number of infection deaths and distress deaths during COVID-19 pandemic,
India, March 18-April 12, 2020
1. Number of infection deaths and distress deaths during COVID-19 pandemic,
India, March 18-April 12, 2020

Source:
See https://coronapolicyimpact.org for the data on
distress deaths and https://www.covid19india.org for the data on
infection deaths.
distress deaths and https://www.covid19india.org for the data on
infection deaths.
While some infection deaths may be unavoidable, distress deaths are
preventable. The fact that the mitigation strategy, and in particular the
extended lockdown, suddenly robbed people of their livelihoods has been widely
reported. While this has been a major cause of distress, and of many deaths, we
would like to examine this more specifically. With this objective in mind, we
have been trying to study these cases to understand the nature of distress.
This has not been an easy task and over the last three weeks that we have been
tracking the information, we had to define new categories to capture emerging
features of these deaths. What did we get to learn from this exercise?
preventable. The fact that the mitigation strategy, and in particular the
extended lockdown, suddenly robbed people of their livelihoods has been widely
reported. While this has been a major cause of distress, and of many deaths, we
would like to examine this more specifically. With this objective in mind, we
have been trying to study these cases to understand the nature of distress.
This has not been an easy task and over the last three weeks that we have been
tracking the information, we had to define new categories to capture emerging
features of these deaths. What did we get to learn from this exercise?
The most significant cause of distress deaths so far has been the
fear of the disease or stigma associated with the COVID infections. A large
number of people who were suspected of infections committed suicide, died in
attempts to escape from miserable conditions in which they were quarantined, or
killed somebody in an attempt to escape. Out of 181 distress deaths recorded until
the time of writing, 50 were attributable to such reasons. Between March 27 and March 30,
when the massive exodus of informal workers happened from cities towards their
native villages, a number of them were run over by trucks and other vehicles
carrying essential supplies. We have recorded 32 such deaths. In Telangana, Tamil
Nadu, Karnataka and Kerala, a number of cases have been reported of alcoholics
dying because of consuming various poisonous chemicals and concotions because
of inability to get alcohol. We have recorded 41 such deaths.
fear of the disease or stigma associated with the COVID infections. A large
number of people who were suspected of infections committed suicide, died in
attempts to escape from miserable conditions in which they were quarantined, or
killed somebody in an attempt to escape. Out of 181 distress deaths recorded until
the time of writing, 50 were attributable to such reasons. Between March 27 and March 30,
when the massive exodus of informal workers happened from cities towards their
native villages, a number of them were run over by trucks and other vehicles
carrying essential supplies. We have recorded 32 such deaths. In Telangana, Tamil
Nadu, Karnataka and Kerala, a number of cases have been reported of alcoholics
dying because of consuming various poisonous chemicals and concotions because
of inability to get alcohol. We have recorded 41 such deaths.
|
Cause
|
Number of Deaths
|
|
Suicide/homicide due to fear/stigma
|
50
|
|
Suicide/death related to alcohol withdrawal
|
41
|
|
Migrants killed in road accidents
|
32
|
|
Death due to exhaustion/hunger
|
20
|
|
Death due to transport blockade
|
13
|
|
Death due to police atrocity/retaliation
|
8
|
|
Honour killings/suicides during lockdown
|
5
|
|
Suicide due to loss of employment
|
4
|
|
Other accidents caused as a result of govt actions
|
4
|
|
Deaths of providers of critical services
|
2
|
|
Sexual assault
|
1
|
|
Stress, depression, trauma because of lockdown
|
1
|
A number of migrants died of exhaustion
or hunger as they attempted to walk hundreds of kilometers to reach their
villages. Even after the initial wave of migrants subsided after the first week
of lockdown, the deaths due to hunger have continued to rise steadily. At the
time of writing this piece, a total of 20 persons were recorded to have died
because of hunger or exhaustion. This includes the report, which came as we
were writing this article, of 5 children who were thrown into the river by
their mother because she could not feed them.
or hunger as they attempted to walk hundreds of kilometers to reach their
villages. Even after the initial wave of migrants subsided after the first week
of lockdown, the deaths due to hunger have continued to rise steadily. At the
time of writing this piece, a total of 20 persons were recorded to have died
because of hunger or exhaustion. This includes the report, which came as we
were writing this article, of 5 children who were thrown into the river by
their mother because she could not feed them.
There has also been a steady rise in
deaths because of police atrocities (8 in total) and transport
restrictions (13). Transport restrictions have resulted in, most importantly, deaths
of patients who were unable to reach hospitals as well as suicides by farmers
unable to transport their produce to the market.
deaths because of police atrocities (8 in total) and transport
restrictions (13). Transport restrictions have resulted in, most importantly, deaths
of patients who were unable to reach hospitals as well as suicides by farmers
unable to transport their produce to the market.
The fact that there are so many different
causes of deaths is noteworthy. The impact of lockdown and restrictions has
been extremely differential across classes, castes and gender. This is also
seen starkly in the data on deaths. There was a recorded killing of a person
who had fled his village after inter-caste marriage to save his live but was
forced to return to the village because of the lockdown. Young people in love
have committed suicides because they were unable to escape the wrath of their
families because of the lockdown. Women in isolation have been killed or forced
to commit suicide because of sexual assaults. A sanitation worker died while
fumigating the streets because the local administration did not think it
necessary to provide the person with mask and other safety equipment. A police
sub-inspector committed suicide because of the prolonged stress caused by
imposing the lockdown.
causes of deaths is noteworthy. The impact of lockdown and restrictions has
been extremely differential across classes, castes and gender. This is also
seen starkly in the data on deaths. There was a recorded killing of a person
who had fled his village after inter-caste marriage to save his live but was
forced to return to the village because of the lockdown. Young people in love
have committed suicides because they were unable to escape the wrath of their
families because of the lockdown. Women in isolation have been killed or forced
to commit suicide because of sexual assaults. A sanitation worker died while
fumigating the streets because the local administration did not think it
necessary to provide the person with mask and other safety equipment. A police
sub-inspector committed suicide because of the prolonged stress caused by
imposing the lockdown.
The dark green colour in Figure 1 refers
to deaths due to accidents caused as a result of government actions. This
category came into being on April 5th when an old woman and two girls died in a
village in Munger because their hut caught fire thanks to lighting of lamps at
9 pm in response to the call by the Prime Minister to do so.
to deaths due to accidents caused as a result of government actions. This
category came into being on April 5th when an old woman and two girls died in a
village in Munger because their hut caught fire thanks to lighting of lamps at
9 pm in response to the call by the Prime Minister to do so.
It has been widely discussed that the
viral infection is, by and large, class and gender blind. This, however, is not
true of the distress that has been caused by the lockdown. Our data clearly
show that a vast majority of distress deaths were from among the poor,
marginalised and vulnerable sections of the society.
viral infection is, by and large, class and gender blind. This, however, is not
true of the distress that has been caused by the lockdown. Our data clearly
show that a vast majority of distress deaths were from among the poor,
marginalised and vulnerable sections of the society.
While most news reports do not provide a
lot of details of the deceased person for us to be able to identify
class/economic status of the person very well, in a large number of reports,
there is some information that broadly indicates the economic/vulnerability
status of the deceased. Of all the reported deaths, we could not decipher the
economic/vulnerability status of the deceased person in 43 cases. Most of these
were unidentified alcoholics. There were also a few others, for example
patients who died because of inability to reach hospitals, where the report
contained no information that would allow us to decipher the status of the
deceased. Since the news reports do not provide adequate information for these
cases, we have classified them as unidentifiable.
lot of details of the deceased person for us to be able to identify
class/economic status of the person very well, in a large number of reports,
there is some information that broadly indicates the economic/vulnerability
status of the deceased. Of all the reported deaths, we could not decipher the
economic/vulnerability status of the deceased person in 43 cases. Most of these
were unidentified alcoholics. There were also a few others, for example
patients who died because of inability to reach hospitals, where the report
contained no information that would allow us to decipher the status of the
deceased. Since the news reports do not provide adequate information for these
cases, we have classified them as unidentifiable.
Even in cases where some information was
available in the news reports, we are able to do only a very broad
characterisation. Of these cases, 131 were identifiable as peasants, rural
workers, urban manual workers or destitutes. The potentially non-poor cases
that are discernible include two public servants, two persons who lived in
apartments in large cities and were therefore unlikely to be poor, and two
foreign travellers.
available in the news reports, we are able to do only a very broad
characterisation. Of these cases, 131 were identifiable as peasants, rural
workers, urban manual workers or destitutes. The potentially non-poor cases
that are discernible include two public servants, two persons who lived in
apartments in large cities and were therefore unlikely to be poor, and two
foreign travellers.
Table 2: Number of
distress deaths of persons belonging to different occupational/economic
categories
distress deaths of persons belonging to different occupational/economic
categories
|
Class
|
Number of Deaths
|
|
Peasants, rural workers, urban wage workers and destitutes
|
131
|
|
Public servant
|
3
|
|
Urban non-poor
|
2
|
|
Foreign traveller
|
2
|
|
Unidentifiable
|
43
|
It is also noteworthy that, while
infection deaths have been concentrated in a few large cities, distress deaths
have taken place all over the country and have been concentrated in smaller
cities, towns and villages. If one excludes Maharashtra, where a large number
of infection deaths have taken place in a few major cities, and Madhya Pradesh,
where a number of infection deaths have taken place in Indore, one finds that
the recorded distress deaths far outweigh the infection deaths (Figure 2). The
strategy of lockdown may be effective in ensuring physical distancing and
isolation in better-off parts of the hotspot cities, the lockdown is not
sufficient to ensure physical distancing in cramped slums in these cities. At
the same time, large parts of rural India are clearly faced with this
continually unfolding socio-economic crisis threatening their lives.
infection deaths have been concentrated in a few large cities, distress deaths
have taken place all over the country and have been concentrated in smaller
cities, towns and villages. If one excludes Maharashtra, where a large number
of infection deaths have taken place in a few major cities, and Madhya Pradesh,
where a number of infection deaths have taken place in Indore, one finds that
the recorded distress deaths far outweigh the infection deaths (Figure 2). The
strategy of lockdown may be effective in ensuring physical distancing and
isolation in better-off parts of the hotspot cities, the lockdown is not
sufficient to ensure physical distancing in cramped slums in these cities. At
the same time, large parts of rural India are clearly faced with this
continually unfolding socio-economic crisis threatening their lives.
Figure 2: Number of distress and
infection deaths in States and UTs other than Maharashtra and Madhya Pradesh,
March 18-April 12, 2020
infection deaths in States and UTs other than Maharashtra and Madhya Pradesh,
March 18-April 12, 2020
Source:
See https://coronapolicyimpact.org for the data on
deaths of COVID-negative persons and https://www.covid19india.org for the data on
deaths of COVID-positive persons.
deaths of COVID-negative persons and https://www.covid19india.org for the data on
deaths of COVID-positive persons.
Figure 3 shows that infection deaths are
high in a few states with hotspot cities such as Maharashtra (such as Mumbai
and Pune), Madhya Pradesh (Indore), and Delhi. At the time of writing this
article, distress deaths are much higher than infection deaths in Assam, Bihar,
Haryana, Jharkhand, Karnataka, Kerala, Odisha, Tamilnadu, Telangana, and Uttar
Pradesh. While there are no infection deaths in Arunachal Pradesh and
Uttarakhand, distress deaths have been reported. While there is a big question
mark on how effective this haphazard response to COVID-19 is in containing
infection deaths, there is no doubt that the distress has spread very widely
and very fast.
high in a few states with hotspot cities such as Maharashtra (such as Mumbai
and Pune), Madhya Pradesh (Indore), and Delhi. At the time of writing this
article, distress deaths are much higher than infection deaths in Assam, Bihar,
Haryana, Jharkhand, Karnataka, Kerala, Odisha, Tamilnadu, Telangana, and Uttar
Pradesh. While there are no infection deaths in Arunachal Pradesh and
Uttarakhand, distress deaths have been reported. While there is a big question
mark on how effective this haphazard response to COVID-19 is in containing
infection deaths, there is no doubt that the distress has spread very widely
and very fast.
Figure 3: Number of distress and infection
deaths, by States and UTs, April 12, 2020
deaths, by States and UTs, April 12, 2020
Source:
See https://coronapolicyimpact.org for the data on
deaths of COVID-negative persons and https://www.covid19india.org for the data on
deaths of COVID-positive persons.
deaths of COVID-negative persons and https://www.covid19india.org for the data on
deaths of COVID-positive persons.
It has been widely discussed that a
highly infectious disease of this kind spreads exponentially, at least until a
vast majority of people are already infected and re-infections do not take
place in a major way. This results in a very fast, and continuously
accelerating, spread of the disease. However, what has not been widely
recognised is that, unless effective public action is taken to control it,
economic distress and mortality due to loss of livelihoods, and the vicious
cycle that it can create, can also compound the deaths caused by the pandemic.
There are at least two reasons why additional mortality because of economic
distress is likely to compound over time. First, the economic factors feed into
each other, and this can create a compounding effect. Secondly, while people
having a certain level of distress can tolerate it for some time, as distress
accumulates, they would lose this ability. A person can go hungry for a few
days, but as undernourishment accumulates, it could reach a point where the person
succumbs to the lack of adequate dietary energy. While the most vulnerable and
most acutely food insecure would be the earliest victims of such distress, over
time, the distress could intensify for a much larger population of persons
which started with moderate levels of vulnerability. It is therefore important
to dispel the misconception that while the mortality due to COVID-19 infections
grows exponentially, the mortality due to economic distress is likely to either
flatten out or at most rise linearly.
highly infectious disease of this kind spreads exponentially, at least until a
vast majority of people are already infected and re-infections do not take
place in a major way. This results in a very fast, and continuously
accelerating, spread of the disease. However, what has not been widely
recognised is that, unless effective public action is taken to control it,
economic distress and mortality due to loss of livelihoods, and the vicious
cycle that it can create, can also compound the deaths caused by the pandemic.
There are at least two reasons why additional mortality because of economic
distress is likely to compound over time. First, the economic factors feed into
each other, and this can create a compounding effect. Secondly, while people
having a certain level of distress can tolerate it for some time, as distress
accumulates, they would lose this ability. A person can go hungry for a few
days, but as undernourishment accumulates, it could reach a point where the person
succumbs to the lack of adequate dietary energy. While the most vulnerable and
most acutely food insecure would be the earliest victims of such distress, over
time, the distress could intensify for a much larger population of persons
which started with moderate levels of vulnerability. It is therefore important
to dispel the misconception that while the mortality due to COVID-19 infections
grows exponentially, the mortality due to economic distress is likely to either
flatten out or at most rise linearly.
We are not trying to understate the risk
of very high mortality because of COVID-19 infections. We are trying to
emphasise that, unless effective measures are taken to control the distress and
mortality due to factors other than the viral infections, the overall level of
mortality could rise at an exponential rate much higher than the rate of growth
of COVID-19 infections.
of very high mortality because of COVID-19 infections. We are trying to
emphasise that, unless effective measures are taken to control the distress and
mortality due to factors other than the viral infections, the overall level of
mortality could rise at an exponential rate much higher than the rate of growth
of COVID-19 infections.
Various experts and public figures have
recommended that dealing with this crisis requires a massive expansion of
social protection including large-scale cash transfers, universal distribution
of free foodgrains, payment of unemployment allowance to NREGA job card
holders, increased public spending, to reduce this distress. By providing a
measure of the socio-economic distress caused by the unpreparedness and
unplanned lockdown, this article highlights the criticality of the need to
undertake such measures without delay. Not only is this distress set to
intensify in the weeks to come, the nature of distress is changing and
unfolding with time. While road accidents claimed many lives of migrants in the
early days of the lockdown, hunger, loss of employment, sexual assaults, fear
and stigma have seen a steady rise. With the extenstion of the lockdown, and
with no signs of the social protection measures being on the anvil at the scale
that this crisis warrants, a more complex socio-economic crisis is set to
unfold.
recommended that dealing with this crisis requires a massive expansion of
social protection including large-scale cash transfers, universal distribution
of free foodgrains, payment of unemployment allowance to NREGA job card
holders, increased public spending, to reduce this distress. By providing a
measure of the socio-economic distress caused by the unpreparedness and
unplanned lockdown, this article highlights the criticality of the need to
undertake such measures without delay. Not only is this distress set to
intensify in the weeks to come, the nature of distress is changing and
unfolding with time. While road accidents claimed many lives of migrants in the
early days of the lockdown, hunger, loss of employment, sexual assaults, fear
and stigma have seen a steady rise. With the extenstion of the lockdown, and
with no signs of the social protection measures being on the anvil at the scale
that this crisis warrants, a more complex socio-economic crisis is set to
unfold.
There is also a great need to
systematically record incidents of distress. While the lockdown has
incapacitated academic scholars and social activists from venturing out for
fieldwork, this responsibility lies squarely on the news media. We hope our
observations would throw light on the the historic responsibility the news
media ought to bear on its shoulders at this time.
systematically record incidents of distress. While the lockdown has
incapacitated academic scholars and social activists from venturing out for
fieldwork, this responsibility lies squarely on the news media. We hope our
observations would throw light on the the historic responsibility the news
media ought to bear on its shoulders at this time.
Vikas Rawal and Karthik A Manickem are
economists and are affiliated with the Centre for Economic Studies and
Planning, Jawahahlal Nehru University.
economists and are affiliated with the Centre for Economic Studies and
Planning, Jawahahlal Nehru University.
Vivek Rawal is a disaster management
expert associated with People in Centre, Ahmedabad.
expert associated with People in Centre, Ahmedabad.
We are grateful to Balan
Thanthayudham, Twitter users @CB_Aman, @thej, @rachelchitra and @_kanikas_, and
various other colleages and friends who have helped in compiling the data.
Thanthayudham, Twitter users @CB_Aman, @thej, @rachelchitra and @_kanikas_, and
various other colleages and friends who have helped in compiling the data.